 
All dives should incorporate appropriate decompression stops to minimize such risks. Breathing gas switches should be carefully planned to avoid such effects and avoid changing diluents when tissues are close to critical supersaturation. This phenomenon is known as isobaric counter diffusion. 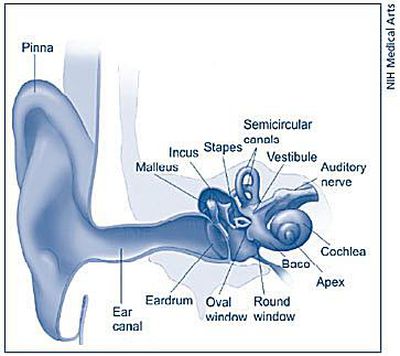
Though the actual mechanism is poorly understood, it is suspected that since helium has a much higher diffusion rate than nitrogen, diffusion of helium into tissues like endolymph that are already close to critical supersaturation could result in bubbling even while at a decompression stop where ambient pressure remains constant. This is most frequently seen in technical/professional divers but can be seen in deep-diving recreational divers as well. Isolated IEDCS is recognized in deep diving with the use of helium-oxygen mixtures, particularly when breathing gas is switched from a decompression mixture containing nitrogen back to a helium-containing mixture (e.g., the diver's bottom mix). This occurs during the ascent of a dive when ambient pressures are reduced at too rapid a rate for the gases to be maintained in solution and be expired via respiration. This dissolved gas is ventilated out of the body during appropriate decompression (a slow ascent to gradually reduce surrounding atmospheric pressure and release super-concentrated nitrogen) through the lungs without significant incident but in DCS, excess dissolved gas is subjected to rapid pressure changes that precipitate gas bubble formation in blood and tissues, causing obstruction and inflammation. This is caused by the diver breathing compressed gas while subjected to high pressures during dives, resulting in super-saturation of the circulatory system with nitrogen due to increased ambient pressure and the compressed gas mix, in accordance with Boyle's law. In general, decompression sickness (DCS) is thought to be caused by the generation of gas bubbles within the vasculature and organ tissues. However, tinnitus and acute sensorineural hearing loss may also be present alone or in any combination. The classic presenting symptom of inner ear DCS is a sudden onset of vertigo. Another suggested mechanism of IEDCS is that patients may also have a right-to-left shunt, suggesting arterial gas embolism (AGE) as a contributing factor if it enters the labyrinthine artery. Inner ear decompression sickness (IEDCS) is an incompletely understood condition observed in compressed-gas divers, likely resulting from precipitation of gas bubbles in the endolymphatic and/or perilymphatic spaces during a quick ascent. The cochlea is the portion responsible for the conversion of mechanical sound waves into action potentials of the auditory nerve, while the vestibular component is comprised of the utricle, saccule, and the semicircular canals and modulates the sense of position and balance. This organ is spiral-shaped and surrounded by a bony exterior and contains a fluid called endolymph, which is responsible for the conduction of sound and changes in position. 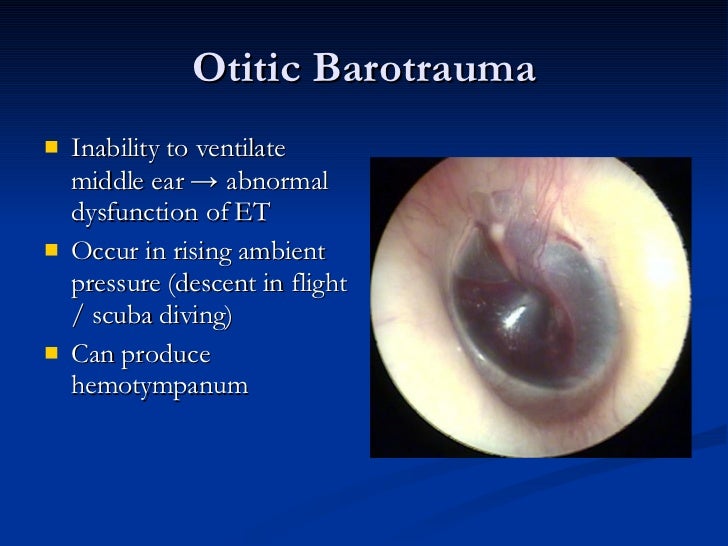
The inner ear consists of the vestibulocochlear organ, which is involved in hearing and one's sense of position and balance. This means that diving-related disorders can present to essentially any hospital, whether inland or coastal, and all emergency and urgent-care clinicians should be aware of signs and symptoms of decompression sickness, in addition to those working in and around formal decompression chambers. However, expansions in the sport have extended recreational dive sites in other bodies of water, including temperate and even polar seas, lakes, quarries, and many others. Originally, divers concentrated most of their dives in warmer coastal regions. 
Recreational scuba diving is an increasingly popular sport globally, with approximately 1.2 million divers worldwide. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
